-
Research & Clinical Studies
Hemodynamics Management with Transesophageal Atrial Pacing
"Bradycardia due to sinus node dysfunction is common in surgical patients under general anesthesia and may produce severe cardiac insufficiency." Atlee, JL, et al. J Cardiothorac Vasc Anesth 7(4), 1993. Abstract
"TAP is widely applicable to anesthetized adults, producing an average 13-16 mm Hg increase in arterial pressure in patients with sinus bradycardia or AV junctional rhythm." Pattison CZ, et al. Anesthesiology 74:854-859, 1991. Abstract
"Since a pacing esophageal stethoscope is usually easy to insert, anesthesiologists can readily accomplish TAP for treatment of sinus bradycardia, AV junctional rhythm and reentrant tachycardia." Roth JV, Brody JD, Denham EJ. Anesth Analg 83:48-54, 1996. Abstract
TAP vs. Anticholinergic Drugs "The slow response time to chronotropic drugs may lead to an inadvertent overdosage (with consequent tachyarrythmias) in an attempt to achieve a more rapid onset of effect, and there have been reports of bradycardias that are resistant to anticholinergic medication. TAP produced more rapid and reliable heart rate changes than either atropine or glycopyrrolate. Bradycardia tended to recur as the effects of chronotropic medications were eliminated, whereas the heart rate remained stable during pacing with the TAPSCOPE." Smith I, Monk TC, White PF. Anesth Analg, 78(2):245-52, 1994. Abstract
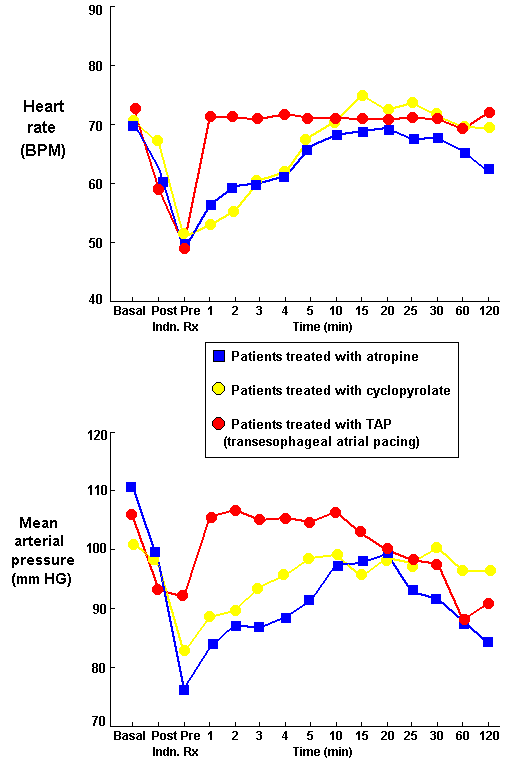
Figure legend: Heart rate and mean arterial pressure values were recorded before and after anesthesia (basal, post), before treatment of bradycardia (pre-Rx), and at the indicated number of minutes after onset of treatment. Summarized from: Comparison of Transesophageal Atrial Pacing with Anticholinergic Drugs for Treatment of Intraoperative Bradycardia. Smith I, Monk TC, White PF. Anesthesia and Analgesia, 78:245-52, 1994.
"CABG patients were randomly allocated to receive treatment for sinus bradycardia (HR < 60 BPM) with either TAP or gallamine. 24/25 TAP patients could be paced at a rate of 70 BPM after SB; cardiac index increased from 1.90 to 2.56 L/min/m2. In the gallamine group, HR increased from 50 to 66 BPM, but CI only increased to 2.2 L/min/m2, and 2 patients developed nodal rhythms. Eight of these patients had peak heart rates over 80 BPM, and two over 90 BPM. The ability to reliably and precisely control heart rate was superior with TAP compared with intermittent bolus dosing with gallamine. Tomichek RC, et al. J Cardiothorac Vasc Anesth 9(3):259-63, 1995. Abstract
Management of Hemodynamics during Cardiac Surgery
"Sinus bradycardia occurred in 15 (of 40) patients after anesthesia induction and was associated with a hypotensive response and a decrease in cardiac output in 10 patients. In these patients, TAP restored diastolic blood pressure and cardiac output to baseline values at TAP rates of 65 and 80 bpm, respectively. Control of heart rate with TAP restores intraoperative hemodynamics to baseline in patients in whom bradycardia and a hypotensive response develop before coronary artery bypass surgery." Hogue CW, et al. Anesthesiology 85(1): 69-76, 1996. Abstract
"TAP method can be applied satisfactorily in children undergoing cardiac surgery. If urgent cardiac pacing must be applied in these patients TAP would be a choice." Sung CS, et al. Chung Hua I Hsueh Tsa Chih (Taiwan), 1995. Abstract
"Transoesophageal pacing is a practical, safe and effective method for emergency cardiac pacing." Paul T, et al. Anaesthesist 42(8):564-6, 1993. Abstract
"Under controlled conditions of general anesthesia for carotid endarterectomy, transesophageal atrial pacing reduced by 40% the amount of phenylephrine needed for blood pressure support and helped in the treatment of disadvantageous sinus bradycardia." Borum SE, et al. J Cardiothorac Vasc Anesth 14(3):277-80, 2000. Abstract
"Although endocardial is via the right and esophageal pacing via the left atrium, we found no significant hemodynamic differences between them. TAP is quicker to obtain with no apparent complications. In these (cardiac) patients, intraoperative bradycardia and hypotension can be improved with the institution of temporary pacing." Rotter SJ, Koehler, D. Anesth Analg 80: SCA78, 1995. Abstract